Op-Ed: Challenging the Hype over Personalized Medicine
By Reef Aldayafleh, MEng ’20 (BIOE)
We grow up being told to embrace our unique characteristics. We customize our phones, clothes, and drinks to our personal preferences. So why not customize our medicine? Advancement in genomics, data collection and artificial intelligence is spurring a new frontier in healthcare: precision medicine (also known as personalized medicine). President Obama launched the Precision Medicine Initiative in 2015 to move healthcare away from the “one-size-fits-all” approach to a more personalized approach of tailored treatments. Researchers are leveraging patient data to develop precise diagnoses and effective treatments.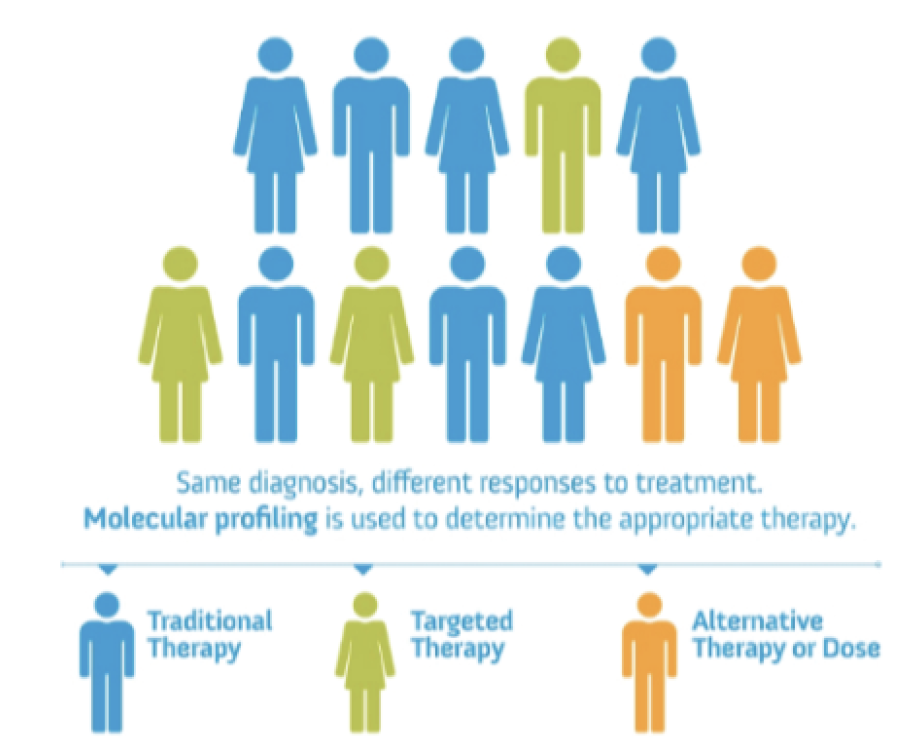
About the author:
Reef Aldayafleh has a passion for exploring the wonders of science, where her curiosity shaped her into an interdisciplinary scientist and engineer. She has an extensive background in research from previous work in nanotechnology, medical devices and life sciences. Reef is currently pursuing a Master of Engineering degree in Bioengineering at UC Berkeley. Prior to attending Berkeley, she received her bachelor’s degree in Bioengineering at UC Merced. She is actively seeking opportunities in innovating and enabling scientific discovery and medical advancements. Connect with Reef.References:
- Fröhlich, Holger et al. “From hype to reality: data science enabling personalized medicine.” BMC medicine vol. 16,1 150. 27 Aug. 2018, doi:10.1186/s12916–018–1122–7
- MacLeod, Katarin & Kraglund-Gauthier, Wendy. (2015). A Case Study of Infusing Technology into Pre-service Secondary Science Teacher Learning: Conceptions and Attitudes While Navigating Changing Digital Landscapes. Journal Of European Education-Avrupa Eğitim Dergisi. 5. 10.18656/jee.24828.
- Rashid, Masturah et al. “Optimizing Drug Combinations Against Multiple Myeloma Using a Quadratic Phenotypic Optimization Platform (qpop).” Science Translational Medicine vol. 10, issue 453. 08 August 2018, doi:10.1126/scitranslmed.aan0941
- Terry, Sharon F. “Obama’s Precision Medicine Initiative.” Genetic Testing and Molecular Biomarkers, Mary Ann Liebert, Inc., Mar. 2015.
- Winslow, Raimond L, et al. “Computational Medicine: Translating Models to Clinical Care.” Science Translational Medicine, U.S. National Library of Medicine, 31 Oct. 2012.
Op-ed: The need for personalized healthcare was originally published in Berkeley Master of Engineering on Medium, where people are continuing the conversation by highlighting and responding to this story.